“You’re trying to solve the unsolvable.”
That was the response we received from the physician we approached with our ReThink idea. Dr. Kellet Letson, VP and Chief of Women’s Health at Mission Health Hospital, was an expert on the complexities of delivering prenatal care to women in rural North Carolina. You could believe him when he said that a group of architects was going to have a hard time solving the frightening problem of infant and maternal mortality in rural America.
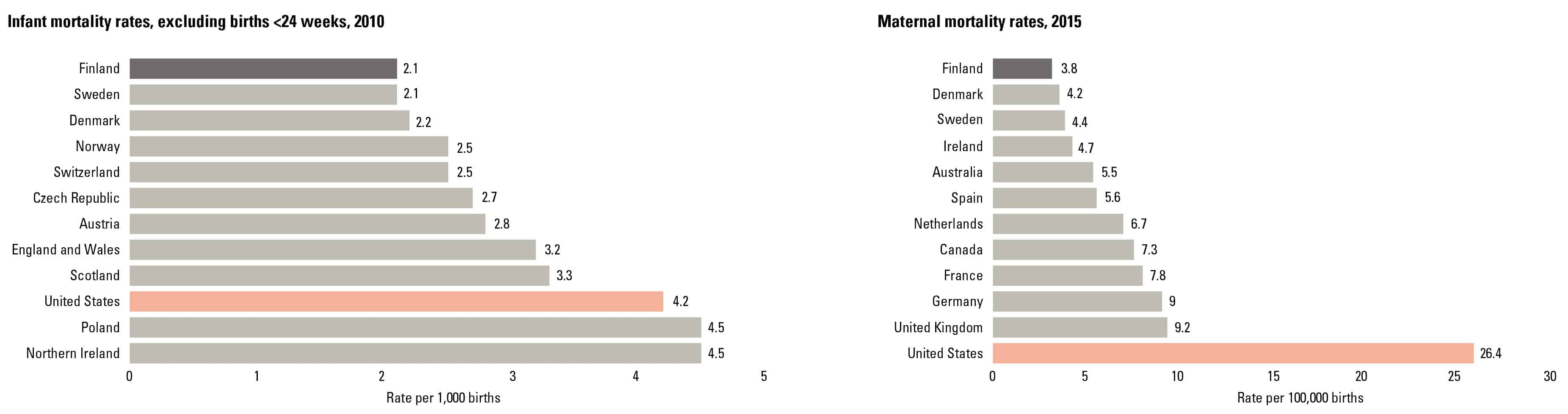
The problem we faced was staggering. The United States has one of the worst rates of infant mortality among first world countries, twice the number of the best ranked country Finland. We also have one of the worst maternal death rates, seven times the rate in Finland. What’s worse, within our country, rural communities face 21% higher infant death rates and 62% higher maternal death rates than urban communities. This problem is alarming and speaks volumes about the state of how healthcare is delivered to these rural mothers.
Before we could design a solution, we first wanted to see how successful countries approached prenatal care. The Finnish government gives women of all socioeconomic levels a ‘maternity box’ that can convert into a crib and is filled with over 50 baby care items. The key is, women can only receive this box after they have their first prenatal clinical visit. In Japan, the approach is group classes and creating small support communities amongst new and experienced mothers. Women with similar due dates go through prenatal and infant care classes together and are encouraged to stay in touch with each other after the delivery, ensuring no mother is isolated or unprepared.

In addition to these approaches of equipping, educating, and embracing these women, Dr. Letson had one more key method: identifying and treating the common pre-existing health conditions that put mothers and babies most at risk. Most rural pregnancies are high-risk due to those health conditions, increasing the chances of infant and maternal death even if they can make the trip to the hospital. The best area of opportunity, said Dr. Letson, was to improve the health baseline of women before they become pregnant.
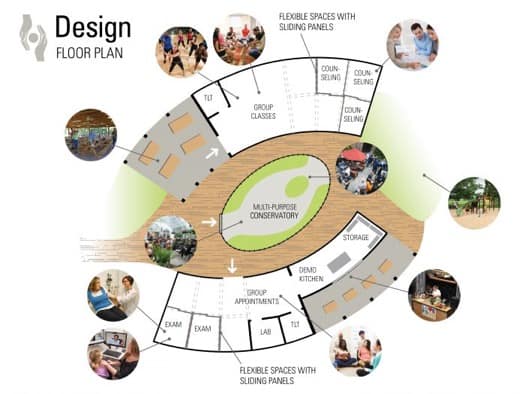
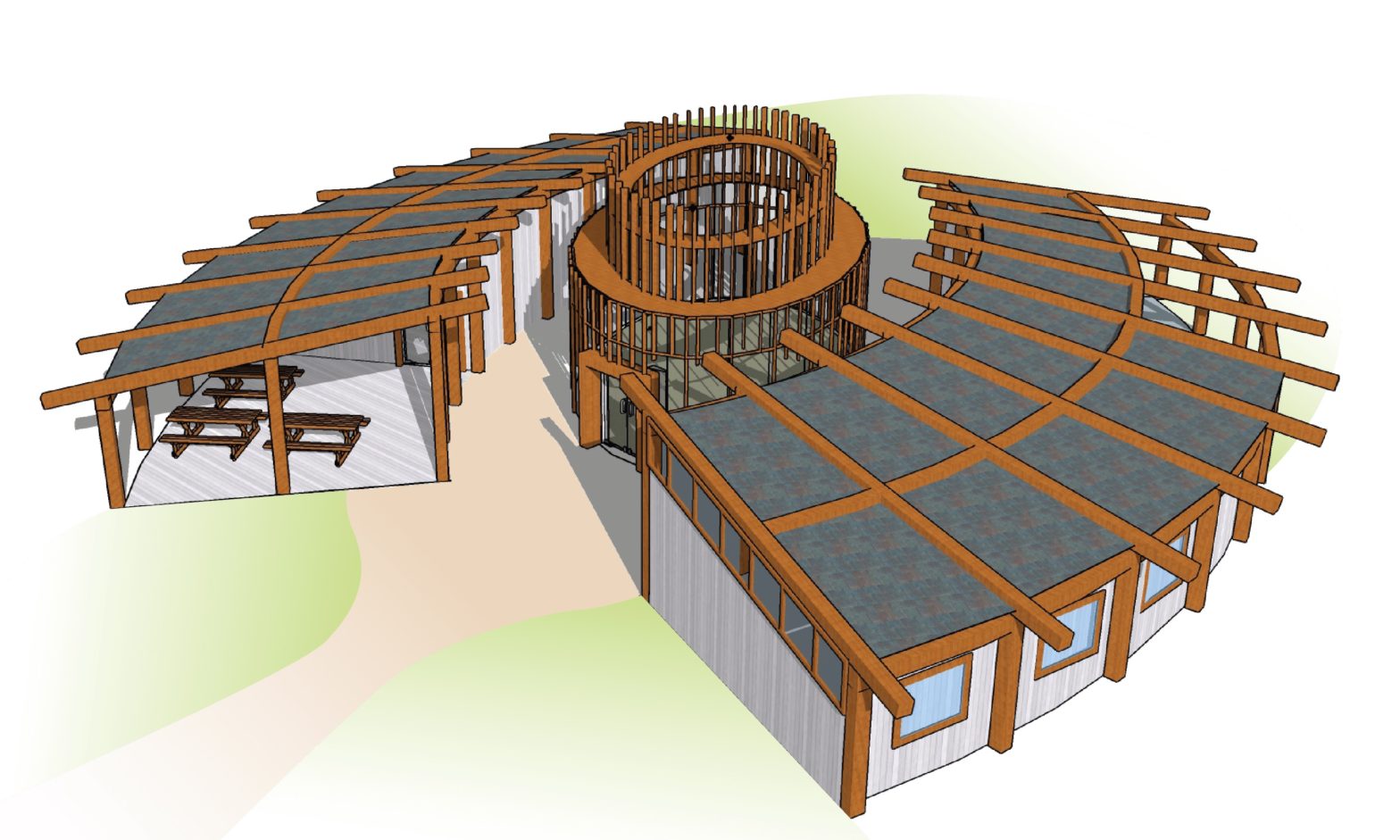
How do we take all this information, and turn it into an architectural solution for such a complex problem? Our idea was to create an adaptable, multipurpose, community-centric, and easily constructed facility that could address the myriad of physical, social, and health-related issues that stand between rural women and a safe delivery. We believed if this design could educate a community to incite change, equip them with the tools they need, and embrace them to elevate hope, we could see true behavioral change and enduring improvements in each woman’s health.
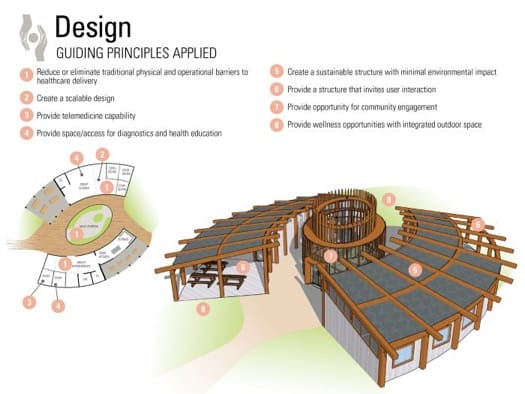
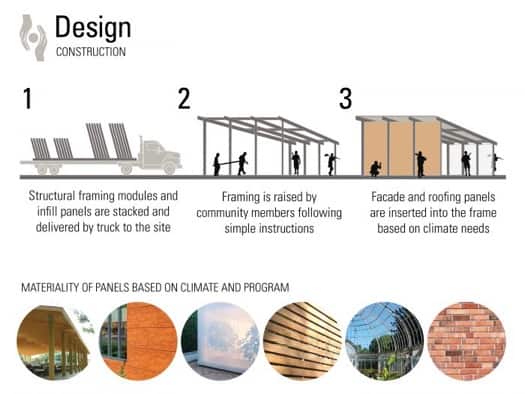
The key characteristic was adaptability: we needed spaces to flex between larger groups and individual needs, between different daily programs, and even between different climates. Rural communities exist everywhere across America: we needed a fabrication system that could keep users either warm or cool, and was simple enough for a layman to construct with minimal instruction.
Our goal for this hypothetical facility was a cycle of continually improving health for rural communities. A facility that provides the education, programs, care, and support is what people need to make and maintain changes to their health behaviors. With fewer pre-existing conditions that cause high-risk pregnancies, rural communities can see better rates of infant and maternal survival year after year.